 
Treatment regimens for BV include oral metronidazole, 500 mg taken twice daily for 7 days metronidazole gel 0.75%, one applicator administered intravaginally daily for 5 days or clindamycin cream 2%, one applicator administered intravaginally at bedtime for 7 days. Amsel's criteria for the diagnosis of BV by wet mount examination are listed in Box 22‐4. 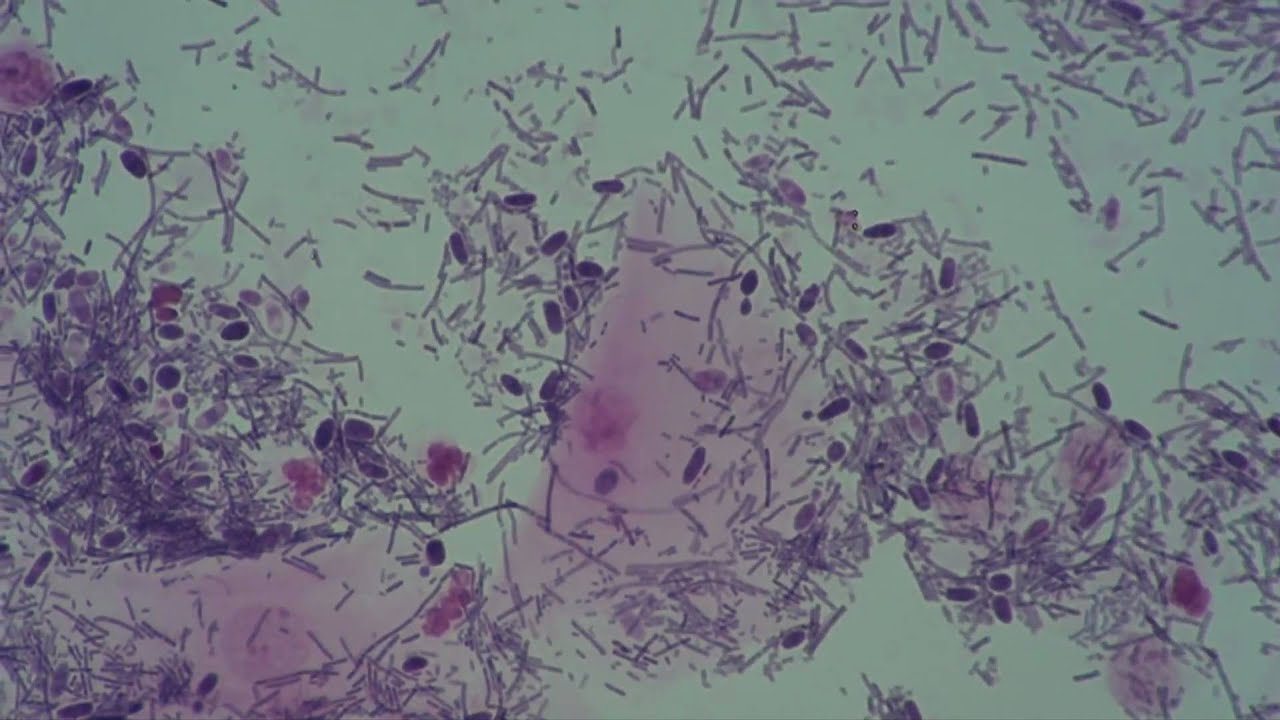
BV is diagnosed by means of wet mount examination. BV may be asymptomatic or may present with a thin, homogenous vaginal discharge and a musty odor. Pregnant women with BV are at increased risk for preterm labor and preterm premature rupture of membranes.Īlthough BV is more common in women with multiple sexual partners, it is not considered an STD because it is also found in celibate women treatment of male partners does not prevent recurrences. Patients with BV are at increased risk for urinary tract infections (UTIs), pelvic inflammatory disease (PID), and vaginal cuff cellulitis at the time of hysterectomy. vaginalis may be detected in 50% to 60% of healthy asymptomatic women. vaginalis have positive results in almost all cases of BV, G. Other organisms commonly involved include Mobiluncus species, Prevotella species, Porphyromonas species, Bacteroides species, and Peptostreptococcus species. BV is typically polymicrobial but is usually associated with an overgrowth of Gardnerella vaginalis and Mycoplasma hominis. Schimpf, in General Gynecology, 2007 Bacterial Vaginosisīacterial vaginosis (BV) is caused by an overgrowth of anaerobic bacteria, replacing the normal lactobacilli and causing an increase in vaginal pH. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
